Medical technology: Is it always the latest and greatest?


By Mylika Scatliffe
Special to the AFRO
The Oxford dictionary defines technology as the “application of scientific knowledge for practical purposes, especially in industry.” Another definition states that “technology is the application of scientific knowledge to the practical aims of human life.” Medicine is a science that constantly evolves and simultaneously stays the same. The construction of the human body doesn’t change. It has suffered many of the same conditions and maladies for centuries. It constantly evolves because technology means we find new ways to treat or even cure old and new diseases. With this evolution even comes new names; diabetes used to be referred to as “sugar.” Parkinson’s disease was called “the shakes.” We learned about leprosy in the Bible, now it’s called Hansen’s disease. Today we survive ailments and acute medical crises that may have killed us as recently as 40-50 years ago.
There are tremendous advances in medical technology. Today, diagnoses, treatment, monitoring, surgical techniques and even how we disseminate and receive information are all more accurate and efficient because of technology. This includes areas of specialty like cardiology, the treatment of lungs and kidneys as well as the tools, machines, and appliances we use for treatment. Even recovery times are greatly reduced.
Dr. Andrew Faber is a board-certified internist with more than 30 years of experience. He’s currently a hospitalist at Lakewood Ranch Medical Center in Lakewood Ranch, Florida, but previously managed inpatient and outpatient care for urban, suburban, and rural patients in upstate New York for many years.
“There is a very important lesson about how to use technology that I think can get lost,” said Faber. “In our country we’re constantly looking for numbers and data and the fact is when we take care of patients, certainly when I do, the patient needs to be the focus and that’s the important lesson that gets lost.” Faber emphasizes that while the advances in all specializations have been tremendous, technology needs to be used in conjunction with other factors. There is a place for it and doctors and other medical professionals must be mindful of how they’re applied. He discussed the use of Magnetic Resonance Imaging (MRIs) as an example. MRI pictures have become so accurate; they find a lot of anatomic issues that might not be problems but lead to unnecessary surgeries and procedures. “Just because you can use something or do a procedure doesn’t mean you should,” Faber stated. Having numbers and data so readily and immediately available may lead to patients and caregivers alike getting bogged down in details. According to Faber, “Details are helpful but mean nothing if a patient doesn’t feel well. For example, a decrease in white blood cell count may be a good sign, but if I check on my patient and he or she feels horrible, we need to consider the numbers and data along with what we find out about how their day went, and what the nurse says about what kind of night they had and put it all together to come up with a plan.”

Dr. Kamala Littleton is an expert orthopedic surgeon with Orthopedics and Joint Replacement at Mercy Medical Center, in Baltimore, Md., and she leads the Women’s Orthopedic Program at Mercy.
Robotics are a relatively recent advance in technology as relates to joint replacement, meaning within the last 5-10 years. With robotic knee replacement, a computerized robot helps the surgeon make accurate bone cuts, and not allowing too much to be cut. The patient has a CAT scan ahead of the surgery, during which decisions are made about what will take place during the procedure. The robot is subsequently able to communicate with the CAT scan results to make sure there is a desirable outcome. All the joint surgeons at Mercy offer robotic knee replacement. While Littleton is respectful of the new technology, she prefers to take a more conservative approach. “In my opinion, knee replacement is more art than science,” stated Littleton; a robot can’t balance ligaments which is important for proper recovery and the success of a knee replacement. Her team respects the technology and believes it will be even better in the future. Littleton has years of specialized training to perform anterior hip replacement as well as MAKO knee resurfacing and knee replacement. Littleton’s innovative procedures and surgical expertise make her a top choice for patients seeking relief from hip, knee, and shoulder pain.
Respiratory therapy, as defined by the American Association of Respiratory Care (AARC), “is the health care discipline specializing in the promotion of optimum cardiopulmonary function, health, and wellness. Respiratory therapists are educated, trained and licensed professionals who employ scientific principles to identify, treat, and prevent acute or chronic dysfunction of the cardiopulmonary system.” If you discuss technology in respiratory care, a respiratory therapist is likely to mention machinery. Dr. Tamara Douglass, Clinical Associate Professor in the Department of Health Sciences at Towson University, in Towson, Maryland, agrees the machines represent the biggest technological change in respiratory patient care.
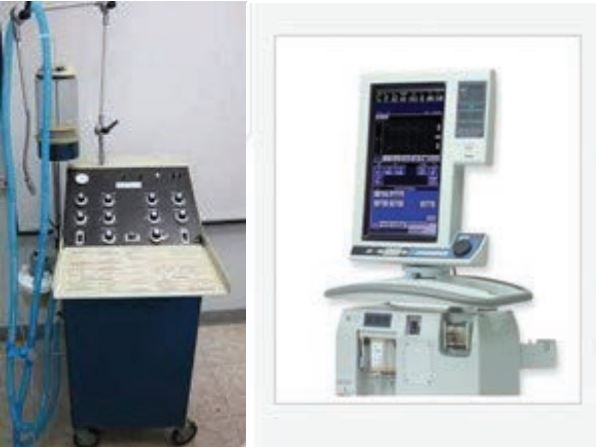
“The advances are so significant that respiratory students now aren’t taught certain types of equipment anymore. They’re still taught most of the same concepts, but some of the machines I learned on, like a MA1 ventilator don’t exist anymore,” said Douglass. The equipment today is all computerized and controlled with push pads; no buttons or knobs. We’re taught all about the body and respiratory system, but today you almost need to spend as much time being technically literate.”
Douglass has been a respiratory therapist for 31 years. She currently specializes in cardiac and pulmonary rehabilitation and sleep studies. Even sleep studies are greatly changed by advances in technology. Sleep studies used to involve reading pages and pages of paperwork generated by brain waves during eight hours of sleep. Now it can all be reviewed live on the computer screen as the patient sleeps.
A Director of Respiratory of Therapy for a large urban hospital (who’s requested not to be identified) also points to the machinery and equipment as the biggest changes in technology for respiratory care. “We used to walk around with calculators but now the machines calculate everything,” he said. He went on to describe how every department is trying to do more with less; less staff, less equipment, less budget, less everything. Machines are used to make up the for the deficit which means machines need to be able to do a lot and do it efficiently. However, he believes a step is lost when relying so much on today’s machinery. “I’ve been doing this for over 30 years, and I’ve noticed that some therapists today don’t want to really learn the craft the way we did. They’re taught to let the machines manage everything, but you still need to be able to know the concepts and make calculations on your own. Machines won’t always know everything. They malfunction, so you still need to learn your craft.” He also explained the need to constantly research and stay abreast of new equipment and techniques. Patients may come to the hospital with their own equipment, and respiratory therapists need to know how to quickly learn and manage unfamiliar equipment. Sales reps are always pitching new equipment and as director he makes decisions on what equipment gets purchased to keep respiratory departments running seamlessly so patient care isn’t compromised.
Advances in medical technology means acquiring and using the latest cutting-edge procedures and equipment, as well as discovering new ways to use current equipment, knowledge, and skill sets. Navigating Covid led to new discoveries such as high flow oxygen as a better treatment for some patients instead of intubation. Laparoscopy and ultrasound, while not new technologies, are constantly evolving and improving. They allow for minimally invasive procedures with less bleeding and quicker and less traumatic recovery. Risks are reduced and patients commonly have surgery and go home within hours.
Then there are devices like the cardiac life vest, a wearable defibrillator that continuously monitors and automatically detects abnormal heart rhythm caused by the heart’s pumping chambers. If necessary, it may deliver an electric shock to restore the heart’s normal rhythm (defibrillation), and perhaps prevent sudden cardiac arrest.
There is absolutely a place for technology in medicine. It promotes the most current and optimal care for patients. There are things being done today that were not imagined as recently as 20 years ago. However, it’s essential to know what your caregiver does best. While reading and researching the latest in treatments, procedures, and devices, remember to research what your doctor does best – whether it’s the latest surgery or a long-established procedure and treatment plan.
Help us Continue to tell OUR Story and join the AFRO family as a member – subscribers are now members! Join here!





